BOSTON — A weathered photograph of a wavy-haired man seated in front of an old-fashioned television.
A handful of miniature American flags draped over a larger U.S. burial flag, folded 13 times into a triangle as dictated by military protocol.
Those treasured items are what Kathy McLeod has left of her late big brother, John Murphy.
Murphy died February 1 at age 80 — following a stay at the for-profit West Roxbury Health and Rehabilitation Center. McLeod said a nursing home administrator told her another resident pushed her brother, causing a fracture in his left thigh bone.
“I loved him,” McLeod told Investigative Reporter and Anchor Kerry Kavanaugh at her Braintree home.
“I just want justice for him.”
McLeod said Murphy, a Vietnam veteran who served in the Marine Corps from 1960 to 1964, loved his family and his country.
He’d often watch over her and her sister, McLeod recalled.
But at some point, with age and the onset of dementia, she became the one looking out for him.
In September 2021, McLeod said Murphy agreed to go to West Roxbury Health and Rehabilitation Center.
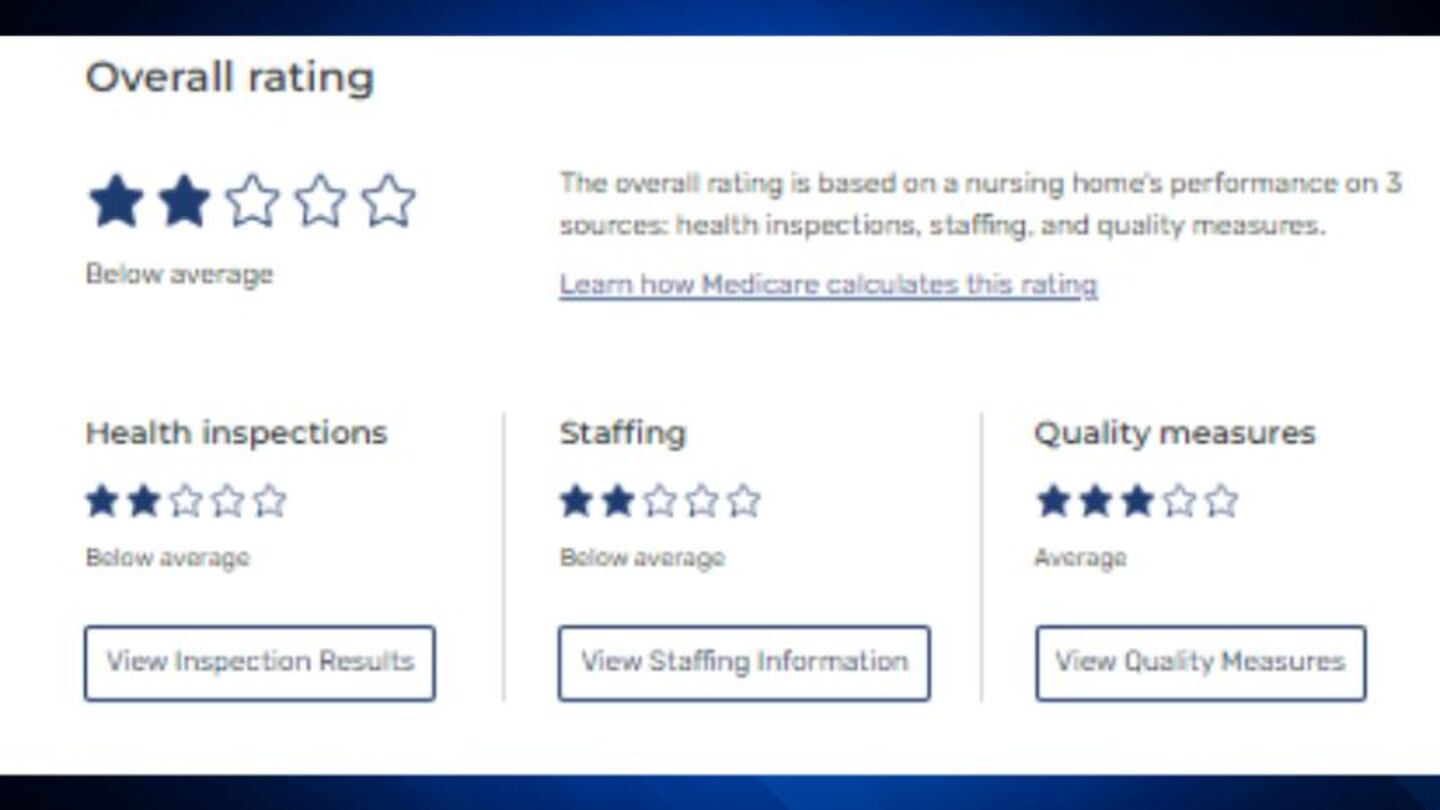
The nursing home has a two-star rating out of five-stars, according to the U.S. Centers for Medicare and Medicaid Services.
And the West Roxbury nursing home was one of two places that the V.A. recommended Murphy go to get the care he needed, McLeod said.
“He was very social,” McLeod said. “When he got in there, he’d shake everyone’s hand in the hallway. He’d pat them on the back.”
But McLeod said within a couple of months, she became concerned about the quality of his care.
“Every time I went in, there was something,” she said.
McLeod recalled: His bed linens weren’t changed. He wasn’t washed properly. He wasn’t eating.
Then, she said, Murphy started to decline.
And he would wander.
“So he started getting, like, he couldn’t work the TV controller,” McLeod said. “He would have a hard time finding his room sometimes.”
NO ANSWERS
McLeod said she regularly met with nursing home administrators about her concerns.
She said she had calls with Bear Mountain Healthcare, a Connecticut-based company that owns multiple nursing homes in Massachusetts, including the West Roxbury facility.
McLeod said she contacted everyone she could think of inside and outside the facility.
“I contacted the ombudsmans,” McLeod said. “There was two of them.”
She also reached out to the Department of Public Health, an elder services agency in Boston, the state Inspector General’s office, the Attorney General’s office, and the VA.
A spokesperson for the state Office of the Inspector General said she cannot confirm or deny any investigations. A spokesperson for the Attorney General’s office said she was working on 25 Investigates’ inquiry.
McLeod provided 25 Investigates with copies of complaints she filed.
But after making all of these calls, and filling out all of these forms, she got no answers.
“Nothing,” McLeod said. “Absolutely nothing.”
In McLeod’s September 22, 2022 complaint to the state Department of Public Health, she said she had observed issues with his care over his past year at the nursing home.
“I have tried to bring these issues up with the staff, with no resolution,” McLeod wrote in her complaint.
“The problem is, there have been four different directors of nurses and four different administrators within this year,” she wrote. “This is unacceptable and it lacks continuity of care.”
She pointed to language barriers and poor attitudes among staff members at the nursing home.
“I have also noticed an increase in the lack of care for my brother, which I consider this to be neglect,” she wrote. “I feel this is discrimination and retaliation against my brother due to my previous conflicts and concerns with the staff.”
“I feel this nursing home needs to be inspected by DPH for the issues of treating patients with attitude and disrespect, as well as lack of good care,” McLeod wrote.
McLeod received an October 3, 2022 letter from the state Department of Public Health acknowledging her concerns about West Roxbury Health and Rehabilitation Center.
“We will receive the concerns in your letter and determine the most appropriate actions to take with this facility,” reads the letter from Steve Reardon, intake supervisor of the public health agency’s complaint unit.
This year, the Department of Public Health has declined 25 Investigates’ numerous requests for sit-down interviews with agency leaders.
A spokesperson for Massachusetts’ Executive Office of Health and Human Services said that “intake surveyors thoroughly reviewed the complaint which was then placed on file.”
“A recertification survey conducted by DPH at this facility in November 2022 found no deficiencies related to the care provided to this resident,” the spokesperson wrote in an email.
McLeod said she never heard back from the state again about that complaint.
BLUNT FORCE TRAUMA
Weeks went by.
On January 10, McLeod got a call from the nursing home saying her brother had fallen.
“What happened was he wandered into a patient’s room,” McLeod said. “He got pushed, fell down, broke his leg, and died. That’s what happened.”
A Boston Police report says police responded to a “radio call for an assault and battery report” at the West Roxbury Health and Rehabilitation Center on January 10.
Nursing staff told police that Murphy was transported to the VA hospital in West Roxbury for an injury to his hip, according to the police report. McLeod said he was transported by ambulance.
“Mr. Murphy was transported… for hip pain after being found on the floor,” reads the report.
A nursing home employee said she had left a patient’s room and found Murphy on the floor at the end of the hall. He told her he didn’t know how he ended up on the floor, according to the report.
One nursing home resident said she witnessed another male resident pushing down Murphy. That male patient told staff he didn’t push Murphy.
Nursing staff told police that it “was not uncommon” for Murphy and the witness to have “bouts of confusion,” according to the police report.
The Boston Police Department didn’t respond to repeated requests for comment.
McLeod said Murphy experienced a massive heart attack as he arrived at the hospital’s emergency room, where he was also found to have a fractured hip.
His hip surgery had to wait until he was more stable, according to McLeod.
Murphy was also positive for COVID-19 — a diagnosis of which she said the nursing home had failed to notify her.
Then on January 15, McLeod said she got a call from the administrator of the West Roxbury nursing home, who told her that her brother fell after another resident pushed him.
Three weeks later, Murphy died at the VA hospital in West Roxbury.
The death certificate lists his cause of death as “complications of blunt force injury of the left lower extremity” as a consequence of a “left femur fracture.”
Murphy’s manner of death is listed as an “accident.”
And his death is described as a “result of injury.”
Murphy’s other significant conditions at the time of his death included Alzheimer’s dementia, chronic obstructive pulmonary disease, and atherosclerotic cardiovascular disease.
After Murphy died, his sister sent another complaint to the Department of Public Health dated March 7.
“Ultimately, my brother, John Murphy, died on 2/1/23, as a direct result of that push, as stated on his certificate of death,” McLeod wrote in her complaint.
In a separate March complaint to Central Boston Elder Services, she said: “I would like the nursing home to be investigated so something like this would not happen to another patient.”
“I feel that this nursing home needs to be inspected by DPH for the...... issues of where they’re treating the patients with their attitude and their disrespect, as well as the lack of good care,” McLeod told Kavanaugh.
“No one ever called me and said: ‘Can I talk to you?’” McLeod said. “Never. And DPH is supposed to be protecting our elderly and do something.”
A spokesperson for the state Executive Office of Health and Human Services said after a “thorough investigation” — McLeod’s March 7 complaint was deemed unsubstantiated.
“DPH routinely conducts inspections of nursing homes and thoroughly investigates all complaints it receives to ensure each facility is meeting its regulatory obligations to provide safe, quality care to residents. If deficiencies are found following an inspection or investigation, DPH works with the facility to ensure all deficiencies are appropriately addressed,” the spokesperson said in a statement.
The Department of Public Health follows up with people who file complaints — if they request updates, according to the spokesperson.
HISTORY OF QUALITY ISSUES
25 Investigates found that nursing home inspectors have uncovered a string of quality and infection control issues at the West Roxbury nursing home over the years.
In recent years, inspectors have also found issues with how staff help residents with bathing and eating — problems that McLeod raised about her own brother’s care.
West Roxbury Health and Rehabilitation Center has below average rankings for health inspections and staffing.
The nursing home provides 3 hours and 5 minutes of nurse staff hours per resident per day — well below the national and Massachusetts average of roughly 3 hours and 45 minutes.
Residents get a half hour of licensed practical and vocational nurse hours per day — roughly half the Massachusetts average of 56 minutes.
And over the past year, three administrators have left the nursing home.
That’s over triple the national and state averages.
The West Roxbury nursing home has paid about $190,000 in fines since 2016 over deficiencies revealed in inspection surveys, according to 25 Investigates’ analysis of state and federal data obtained through public records requests.
That includes a roughly $134,000 fine in 2016 when the nursing home failed to meet fire code standards requiring fire drills and upkeep.
The nursing home also paid a $46,000 fine in October 2020 and another $9,750 fine in November 2022.
In October 2020, inspectors found a resident with milk allergies ended up in the hospital after the nursing home fed them milk, according to inspections obtained by 25 Investigates through a public records request.
Also in October 2020, inspectors found that staff failed to follow infection control procedures.
Inspectors found staff let a transport driver enter the facility without doing a screen for COVID-19 symptoms, according to an inspection report.
In November 2022, inspectors found hygiene issues at the nursing home again: two CNAs were observed passing breakfast trays with their facemasks below their noses. And when a surveyor asked another aide why he wasn’t wearing a mask, the aide took a “wrinkled fold-up mask out of his pocket and put it on.”
Surveyors found the nursing home failed to provide showers for two out of 21 sampled residents — including a resident with severe cognitive impairment who depended on staff for bathing.
“During an interview on 11/08/22 at 11:34 A.M., Resident #39 said he/she does not get showers and would love to have one,” the inspection reads. “Review of the shower schedule for the unit indicated Resident #39 was scheduled to have a shower weekly on Sundays.”
But inspectors said nursing records failed to document that the resident was showered for three months: from September to November 2022.
An aide who was caring for the resident in November told inspectors the resident was “scheduled for a shower this week.”
The aide said, “her day was too busy to give Resident #39 a shower.”
“CNA #2 was unable to say the last time Resident #39 had been given a shower,” the inspection report says.
The interim nursing director told inspectors the resident “will often refuse care.”
But inspectors reviewed the resident’s care plan and medical records and said there wasn’t any documentation the resident had refused showers.
Another November 2022 survey found the nursing home failed to follow care plans for five residents — including residents who didn’t have a call light in reach and who didn’t get needed help with eating.
Inspectors in November 2022 found the nursing home failed to follow federal regulations that require nursing homes to come up with plans to fix ongoing issues.
“The facility does not conduct audits or collect data to demonstrate they are attempting to resolve issues,” reads the inspection report.
The nursing home’s administrator told inspectors: “‘I understand, we are identifying issues, but do not have hard data to show we are looking at that. And I eyeball things to make sure they are fixed.’”
West Roxbury Health and Rehabilitation Center also faced state-level fines for failing to ensure staffers were vaccinated and/or boosted, according to enforcement data obtained by 25 Investigates through a public records request.
State records show the West Roxbury nursing home faced a $50 fine for one staffer in October 2021 and three separate $1,400 fines over four staffers between February and May 2022.
FIGHT FOR ANSWERS
For months, 25 Investigates has heard from family members who say they too asked for help for loved ones in nursing homes across our state – and got nowhere.
“What happened?” Crystal Johnson, whose mother died in January 2021 after receiving care at Sterling Village nursing home in central Massachusetts.
Johnson said she never got records from Sterling Village nursing home about what happened to her mom. She’s instead had to rely on hospital records. Sterling Village hasn’t responded to 25 Investigates’ requests for comment.
“How did these things happen?” Johnson said. " Why is there no documentation?”
Patricia W., whose niece has received care at Mattapan Health and Rehabilitation Center, said she has struggled to get answers about flooding and bugs she’s witnessed at the nursing home.
Patricia — who declined to use her last name over fear of impacting her niece’s care — provided 25 Investigates with pictures of dirty living conditions that left her worried for her niece’s wellbeing.
Mattapan Health and Rehabilitation Center is also owned by Bear Mountain Healthcare.
“Nope, I haven’t heard from anybody,” she said.
In 2019, nursing home inspectors found “rodent droppings and dead flies on a window sill that was next to serving utensils and spices” during a tour of Mattapan Health and Rehabilitation Center’s kitchen.
And in February 2022, inspectors found “large quantities of rodent droppings on the floor” of one room — along with an unidentified “black substance” smeared throughout the second-floor residential care unit.
And Mary Addesa, of Dorchester, said her late mother suffered from lack of hygiene, medical and rehabilitation treatment after entering a Stoneham nursing home in early 2021.
“There’s nothing you can do that’s ever going to bring any of our loved ones back,” Addesa said. “But you sure can make a change, give some consequences.”
Sandra Harris, state president of AARP Massachusetts, isn’t familiar with these individual cases — but said it’s clear the nursing home industry needs an overhaul.
“This industry has been in crisis for some time,” she said.
“First of all, in staffing,” Harris said. “Number two, in infection control. Number three is just being transparent and being held accountable.”
After numerous calls and emails, Kavanaugh tried to find an administrator at the West Roxbury nursing home in person.
An administrator told her: “Yeah, I don’t know… I would prefer not to be on camera, though.”
Officials with Bear Mountain Healthcare have not responded to 25 Investigates’ multiple requests for comment left by email, phone, and on the company’s website.
McLeod said it’s wrong that she never got any follow-up from the Department of Public Health after lodging a complaint concerning her brother’s death.
“This nursing home needs to be held accountable for their actions of abuse and neglect of elders,” she wrote in her March complaint.
“It’s time someone stood up for these people,” she told Kavanaugh.
Download the FREE Boston 25 News app for breaking news alerts.
Follow Boston 25 News on Facebook and Twitter. | Watch Boston 25 News NOW
©2023 Cox Media Group